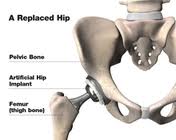
A Guide for Patients with Metal-on-Metal Total Hip Replacements
The Mass General Center for Metal-on-Metal Total Hip Replacement provides state-of-the-art comprehensive care to patients with metal-on-metal total joint replacements and conducts cutting-edge research. Our physicians and researchers have transformed basic discoveries into clinical practice and provide critical evaluation for and specific advice for metal-on-metal implants.
Because some patients with Metal-on-Metal (MoM) hip replacements develop unexplained pain, and because a few develop abnormal tissue reactions to the wear of the implants and require a reoperation, we established a Center that patients could rely on for comprehensive clinical evaluation.
In the majority of cases, conventional pre-operative tests (plain radiographs and standard blood tests) do not reveal any abnormality. Thus, the ordinary follow up evaluation may be of limited value. The mission of Mass General Center for Metal-on-Metal Total Hip Replacement is to provide excellence in clinical care to MoM patients by integrating various specialized tests (analysis of blood samples for metal ions, and imaging studies) in order to establish if an adverse reaction to MoM THR implants is present and to formulate the best way to treat these problems.
via Patient Guide to Metal-on-Metal Total Hip Replacements – Massachusetts General Hospital, Boston, MA.






![MPj03857930000[1]](https://hipsterclub.com/wp-content/uploads/2011/05/mpj038579300001.jpg?w=214&h=300)